Ontario’s healthcare system continues to operate under sustained pressure including crowded emergency departments, delayed admissions, and ongoing workforce shortages. While solutions are often framed around adding resources, an equally critical opportunity lies in how we better understand and optimize the workforce we already have. Registered Practical Nurses (RPNs) are central to that solution.
A forthcoming WeRPN report offers a deeper, evidence-informed look at the impact of the RPN role—highlighting contributions that extend beyond individual patient interactions to influence how the entire system functions.


For decades, Registered Practical Nurses (RPNs) have been an essential part of Ontario’s health care system. Every day, in profound ways, they are present at some of the most important and meaningful moments in people’s lives. But, unfortunately, too often their role continues to be misunderstood, underestimated, or overlooked.
This report was commissioned to change that.
Dianne Martin,
CEO, WeRPN
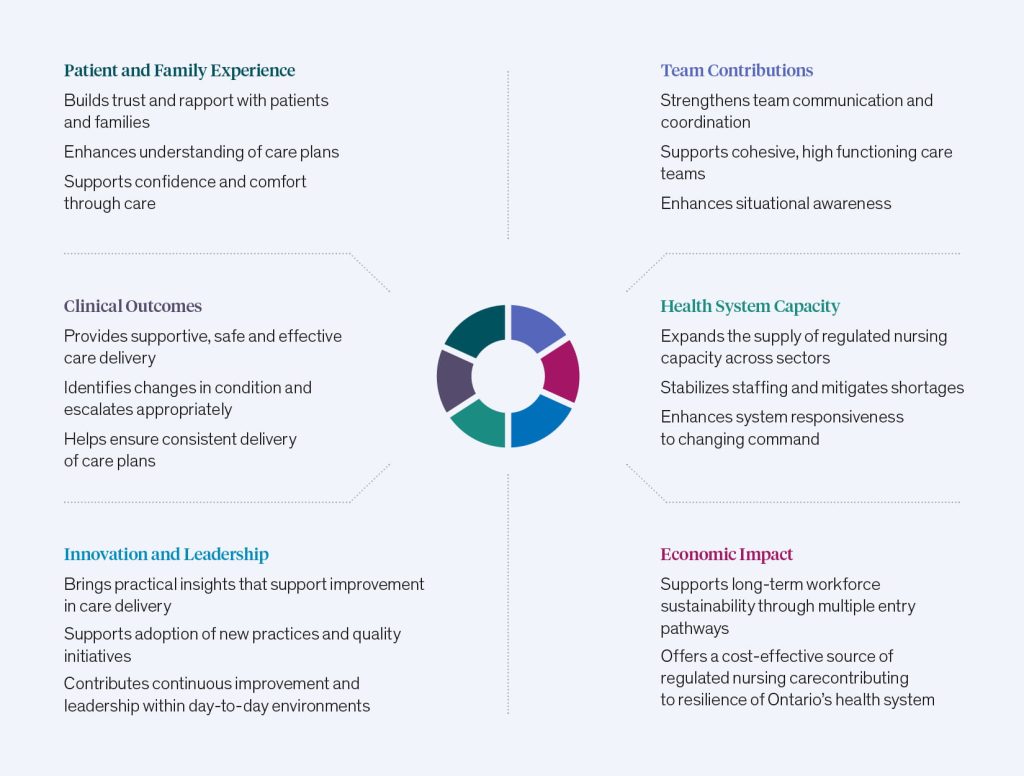
The report introduces a value framework that captures how RPNs contribute across six interconnected domains: patient and family experience, team contributions, clinical outcomes, innovation and leadership, health system capacity, and economic impact. Together, these domains reflect not only what RPNs do, but how their work strengthens care delivery at every level.
At the patient level, RPNs are often the consistent presence in care. Their sustained interactions build trust, support communication, and create continuity which are all factors that shape how care is experienced day-to-day. At the team level, RPNs are integral to coordination, translating care plans into action and ensuring that information flows effectively across providers.
These contributions have direct implications for system flow.

RPNs’ proximity to patients allows for early identification of changes in condition, timely communication, and rapid response within teams. In practice, this reduces delays in care, prevents avoidable escalations, and supports smoother transitions across units and care settings. In high-pressure environments, these seemingly small, continuous actions are what keep the system moving.
The report also highlights the role of RPNs in supporting clinical quality and innovation. Through ongoing assessment, monitoring, and collaboration, RPNs contribute to safe, high-quality care. At the same time, their closeness to day-to-day practice positions them to identify inefficiencies and drive practical improvements which often leads to changes that enhance both patient experience and team functioning.
From a system perspective, RPNs are a critical lever for expanding capacity. They increase the supply of regulated nursing care and enable more flexible staffing models that align provider competencies with patient needs. This alignment is essential to reducing hospital strain—ensuring that higher-acuity resources are used where they are most needed, while maintaining quality across the continuum of care.
Importantly, this is not about substitution but optimization.
When RPNs are intentionally integrated and their role is clearly understood, teams function more effectively, resources are used more efficiently, and care delivery becomes more sustainable. When they are not, the system risks creating unnecessary bottlenecks and underutilizing a highly skilled workforce.
As Ontario continues to navigate growing demand, the path forward is clear. Strengthening the system will depend not only on adding capacity, but on recognizing and fully leveraging the contributions already within it.
RPNs are not an adjunct to the system—they are a foundation of it.


